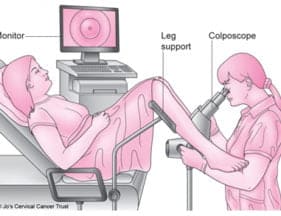
Colposcopy is a type of cervical cancer detection test. It is a diagnostic procedure in which cervix ( opening of the uterus ), vagina and vulva can be visualized in magnified, illuminated view. Many precancerous and cancerous lesions of these areas can be detected by this examination. The main goal of colposcopy is the early detection of cervical cancer and treatment.
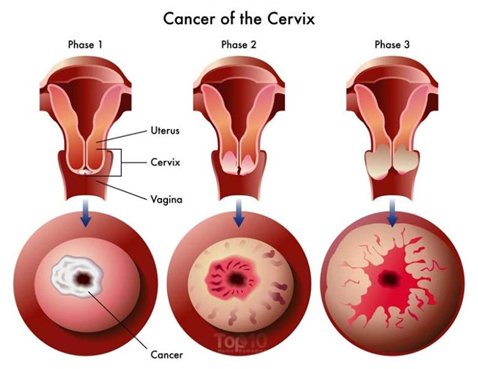
Cervical cancer is cancer of the cervix (lowermost opening of the uterus in the vagina).
Precancerous lesions in cervical cells are present years before full-blown cancer. These early changes in cells are called Dysplasia or CIN (cervical intraepithelial neoplasia). If early changes in cells are detected, cervical cancer can be prevented.

According to WHO data, India contributes to 1/3rd of the global burden of deaths due to cervical cancer.
Currently, it is considered to be No. 1 cancer in India.
In India, every seven minutes, one woman succumbs to cervical cancer death. Daily over 200 women die of this cancer.
Most important risk factor for having cervical cancer is having one of the high-risk HPV infection. Reasons for getting HPV infections are unknown but HPV easily spreads from sexual skin to skin contact with the person infected by it.
Besides HPV following are other risk factors
• History of dysplasia of cervix, vagina or vulva.
• Family history of cervical cancer.
• Immunity lowering conditions like HIV/AIDS make it difficult to fight HPV.
• Other sexually transmitted infections like Chlamydia.
• Age is also a factor. The average age of diagnosis of cervical cancer is around 48years.
Infection with HPV does not usually show any symptoms. Symptoms suggest that disease development has already started. However, some symptoms may include:
• Continuous vaginal discharge( it may be pale, watery or pink, bloody, brown or foul smelling).
• Bleeding or spotting after coitus.
• Bleeding after menopause.
Any of these symptoms warrant examination by a gynecologist.
Regular check-ups with PAP, LBC and HPV DNA tests.
• PAP smear examines the stained sample of cervical cells taken by spatula during per speculum examination. Cell abnormality, infections, and inflammation can be detected by it.
• LBC: Liquid-based cytology, covers all the cells taken by brush from the cervical surface, giving wider exposure to cell abnormality detection.
• HPV DNA test detects high-risk variants of HPV infection.
• It is recommended that every woman of age 30years and above should do this test.
• If the test comes negative, it shows the negligible risk of cervical cancer with 99.7% certainty for the next few years. The test can be repeated after 3-5 years. If positive, then there is an increased risk of pre-cancer or cancer in the future.
Colposcopy is done for:
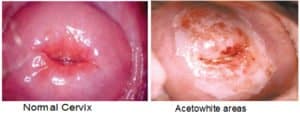
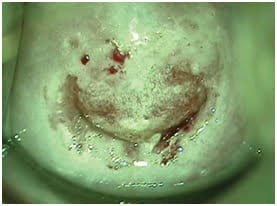
• Cervical cancer screening tests (PAP, LBC, HPV/DNA) showing abnormal changes in cells of the cervix. Colposcopy provides more information about abnormal cells.
• Cervicitis (Inflamed cervix with continuous vaginal discharge).
• Genital warts on the cervix.
• Non-cancerous growths as polyps.
• Abnormal vaginal discharge.
• Abnormal bleeding.
If the only colposcopy is done without biopsy, there is no discomfort on completion of the procedure.
If a biopsy is performed, pain and discomfort may last for 1-2 days for which medications are provided.
Mild vaginal spotting or brown discharge may be present for a few days.
It is advisable to avoid vaginal tampons, sex or douche during the cervical healing period.
What are options available for management of precancerous cervical lesions diagnosed by colposcopy?
Treatments available for significant lesions include:
• Cryotherapy.
• LEEP (Loop electrical excision procedure.
• Laser ablation